
State immunization information systems (IIS), also known as immunization registries, are population-based databases that record vaccinations administered by participating health care providers in a given state (1). Most states require providers to…

Patient use of their health information accessible to them through online tools (e.g., patient portals and smartphone apps) can help empower them to make informed decisions about their health and track progress on health-related goals, potentially…

The 2020 ONC Cures Act Final Rule implements provisions of the 21st Century Cures Act to require secure access to patient health information through application programming interfaces (APIs), with the goal that more patients would be able to access…

Social determinants of health refers to social factors and physical conditions of the environment in which people are born, live, learn, work, and play (e.g., employment, education, social and community context) that affect health and quality-of-…

As of January 2022, eligible hospitals and critical access hospitals (CAHs) that participate in the Centers for Medicare & Medicaid Services’ (CMS) Medicare Promoting Interoperability (PI) Program are required to electronically submit data to…

Prior to the coronavirus disease 2019 (COVID-19) pandemic, adoption of telemedicine was slow and its usage was rare [1]. However, during the pandemic, usage of telemedicine increased dramatically with physicians using a number of telemedicine tools…

Interoperable exchange of health information or “interoperability” is critical for delivering appropriate care, reducing health care costs, and making health care more efficient (1-3). ONC is executing on a number of health IT provisions from the…

Electronic prescribing of controlled substances (EPCS) enables clinicians to securely transmit prescriptions for controlled substances to a pharmacy (1). Prescription drug monitoring programs (PDMPs) are electronic databases that contain patient-…

Hospitals play an important role in support of public health functions by contributing timely and accurate data to state and local public health agencies (PHAs). However, the COVID-19 pandemic revealed substantive gaps in our public health…

Over the past several years, federal policy levers have been enacted to increase patient’s access to their health information. In 2014, hospitals were incentivized by the Centers for Medicare & Medicaid Services (CMS) Electronic Health Record (…

The COVID-19 pandemic exposed gaps in the nation’s public health infrastructure, including a need for increased electronic exchange of patient health information between health care providers and public health agencies (PHAs) (1). Physicians play a…

Increasing interoperable exchange using certified health electronic health records (EHRs), and other information technology (IT) has the potential to improve health outcomes (1), enhance effiency (2) and reduce costs (3). Towards that end, public…

Electronic prescribing of controlled substances (EPCS) technology enables clinicians to securely transmit prescriptions for controlled substances to a pharmacy (1). In 2018, the Substance Use Disorder Prevention that Promotes Opioid Recovery and…

In May 2020, the Office of the National Coordinator for Health IT (ONC) finalized federal rulemaking that aimed to increase the access, exchange, and use of electronic health information by patients and their caregivers (1). This rule implements key…

Amidst a global pandemic, the need for efficient exchange of electronic health information between
hospitals and public health agencies has never been more critical. To ensure public health agencies have
timely and complete data…

A patient’s access to their health information is required and reinforced through multiple federal policy
levers. The Office of the National Coordinator for Health Information Technology (ONC) Health IT
Certification Program certifies health…
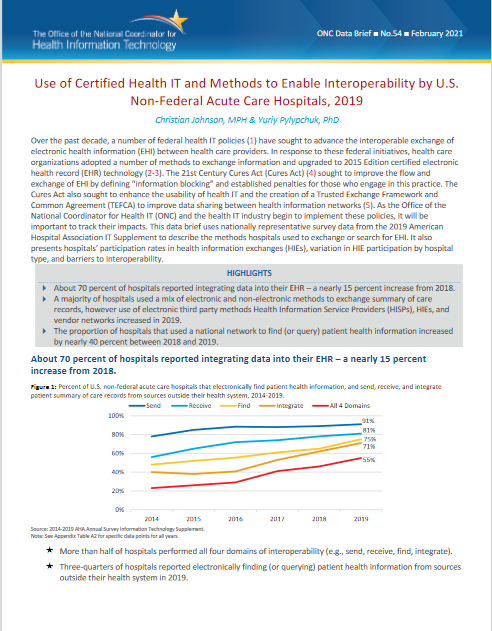
Over the past decade, a number of federal health IT policies (1) have sought to advance the interoperable exchange of
electronic health information (EHI) between health care providers. In response to these federal initiatives, health care…
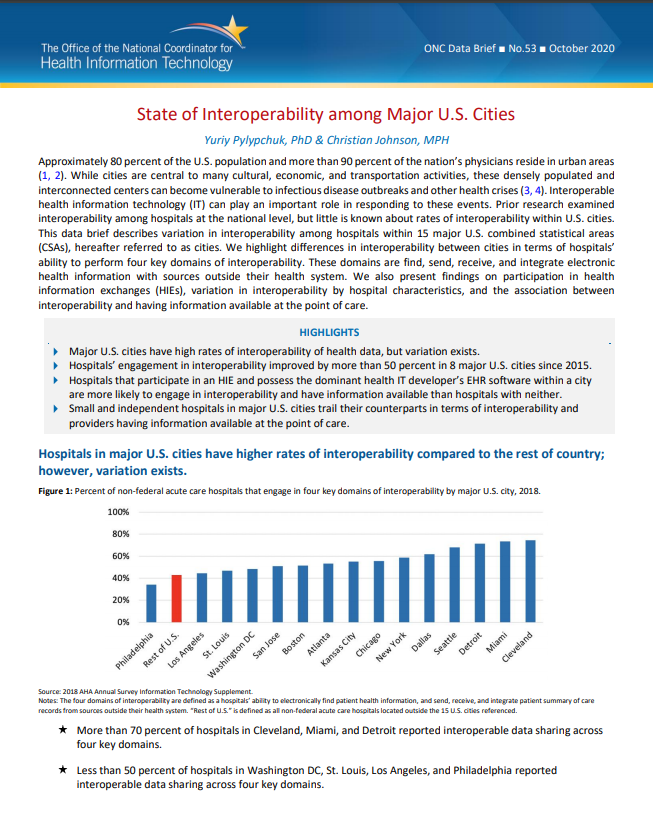
Approximately 80 percent of the U.S. population and more than 90 percent of the nation’s physicians reside in urban areas (1, 2). While cities are central to many cultural, economic, and transportation activities, these densely populated and…


